Plantar Fasciitis treatment in Thane | Kalwa | Parsik Nagar
Dr. Vivek Maurya (MBBS, M.S Orthopaedics, F.I.F.A.S)
(Consultant Orthopaedic Foot and Ankle Surgeon)
ORTHO WELLNESS CLINIC
Shop 12, Building-2, Vastu Anand Society, Parsik Nagar, Kalwa, Thane(W) 400605
Heel pain is one of the most common foot complaints among adults. Many patients assume it is "just strain" or a temporary issue. But when the pain is sharp with your first steps in the morning or returns after long hours of standing, it may be plantar fasciitis.
If you are experiencing persistent heel pain in Thane or Kalwa, early specialist evaluation can prevent chronic discomfort and long-term complications.
What is Plantar Fasciitis?
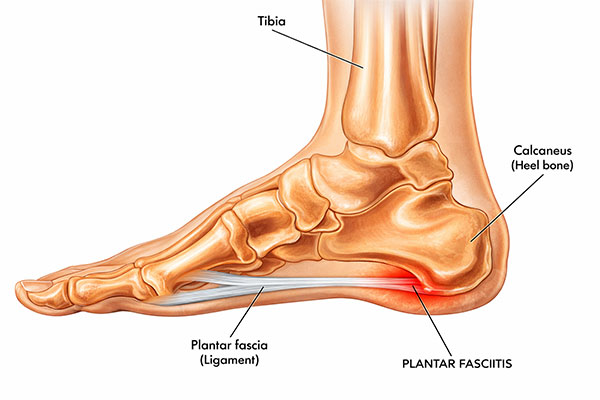
Plantar fasciitis is the inflammation of plantar fascia and is one of the most common causes of heel pain seen in orthopaedic practice, especially among runners, athletes, and individuals who stand for prolonged hours.
Why does Plantar Fasciitis occur?
What Happens Microscopically?
- Collagen disorganization
- Microtears at the insertion site
- Thickening of the plantar fascia
- Reduced vascularity
- Degenerative changes rather than acute inflammation
Typical site of pain is at the medial heel.
What are the symptoms of Plantar Fasciitis?
The hallmark symptom is sharp heel pain typically with the first step in the morning. But every heel pain is not Plantar Fasciitis
Treatment
Most patients (90–95%) improve with conservative treatment within 2 months. However, refractory or chronic cases may take longer.
Frequently Asked Questions
1) Why does Plantar fasciitis cause more pain in the morning?
In sleep the plantar fascia tightens. Upon getting up the fascia stretches, thereby causing pain. Hence, night splints are recommended as they keep plantar fascia stretched at rest.
2) Can Plantar Fasciitis cause pain all day long?
The classical presentation is early morning pain or pain after prolonged rest. However, in chronic cases there maybe discomfort throughout the day.
3) How long does Plantar fasciitis last?
With proper treatment most patients improve in about 2 months period. However, refractory and chronic cases may last longer and need to be evaluated by a Foot and Ankle Orthopaedic surgeon.
4) How to diagnose Plantar Fasciitis?
Diagnosis is clinical based on symptoms and examinations. Radiographs and MRI may be additionally needed in severe cases. Hence, consulting a specialist is of utmost importance.
5) Does heel spur lead to Plantar Fasciitis?
Heel spur is a secondary reaction due to chronic Plantar Fasciitis. It is not the cause but an after-effect of Plantar Fasciitis.
6) What is the best treatment for Plantar Fasciitis?
Ideal treatment is highly individualized and is usually a combination of stretching exercises, activity modification, proper footwear and anti-inflammatory medications. Staged physiotherapy and regular follow ups may be needed.
7) Do shoe inserts or in-soles help?
Yes. They provide a cushioning effect and can help relieve the strain on plantar fascia. However, custom orthotics may sometimes be needed.
8) Are steroid injections safe?
They may provide symptomatic relief in severe cases but the effect may be short-lived and Plantar Fasciitis may recur. Frequent injections are avoided as it may lead to weakening and rupture of fascia. Hence, they must only be used under an expert guidance.
9) Can weight gain lead to Plantar Fasciitis?
Though not the main cause, increased body weight places additional strain on plantar fascia and can aggravate the condition.
10) Who is at risk for developing Plantar Fasciitis?
People who stand for long hours like workers, teachers, medical professionals etc are at increased risk. Also runners, athletes or people with flat feet/ high arch are predisposed to develop Plantar Fasciitis.
11) Is Plantar Fasciitis a genetic condition?
No. It is not transmitted genetically. However, your foot type and body mechanics may have a familial inheritance leading to increased predisposition for certain foot conditions including Plantar Fasciitis.
12) Is surgery required for Plantar Fasciitis?
Maybe needed in advanced or refractory stage (3-5% of the cases). It is considered only when there is no relief in pain despite proper conservative management for 6-12 months.
13) Can Plantar Fasciitis recur again?
If improperly treated Plantar Fasciitis is known to recur.
14) Can both feet be affected?
Though not a rule, but both feet can be affected.
15) Whom should I consult for Plantar Fasciitis?
Every heel pain is not Plantar Fasciitis. Foot and ankle injuries require specialized understanding of joint biomechanics. A dedicated foot and ankle surgeon provides more precise diagnosis and advanced surgical techniques compared to general treatment.
If you are experiencing persistent heel pain in Thane, Kalwa or Parsik Nagar consult a foot and ankle specialist for proper diagnosis and treatment of plantar fasciitis. Timely care prevents chronic complications and long-term discomfort.
Book a Consultation at Ortho Wellness Clinic
Heel pain is treatable. With the right approach, most patients return to normal activity without surgery.
Schedule a consultation at Ortho Wellness Clinic, Thane for comprehensive foot and ankle evaluation and evidence-based treatment.
Early care. Accurate diagnosis. Long-term relief.
Dr. Vivek Maurya
(MBBS, M.S Orthopaedics, F.I.F.A.S)
USA trained Consultant Orthopaedic Foot & Ankle Surgeon
Dr. Vivek Maurya is a dedicated Orthopaedic Surgeon with focused expertise in Foot and Ankle disorders. With advanced fellowship training and years of clinical experience, he specializes in the precise diagnosis and management of complex heel pain, sports ankle injuries, deformities, and diabetic foot conditions.
At Ortho Wellness Clinic, his approach goes beyond symptomatic relief. Each patient undergoes a detailed clinical and biomechanical evaluation to identify the true cause of pain — ensuring targeted and long-lasting treatment outcomes.
For consultation: 9702827531
Visit to know more: drvivekmauryaortho.in
ORTHO WELLNESS CLINIC
Shop 12, Building-2, Vastu Anand Society, Parsik Nagar, Kalwa, Thane(W) 400605
Book Appointment →